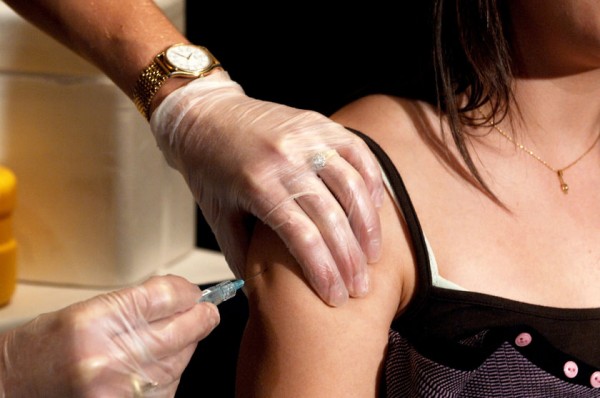

Parents may not want to think about their child being sexually active. But in the case of the vaccine for human papillomaviruses (HPV), the issue isn’t whether or not a child is sexually active now—it’s whether or not they will be protected in the future.
Even though the HPV vaccine is one of the only vaccines that prevents cancer, fewer than 50 percent of adolescent girls in California were fully vaccinated against HPV in 2011. Vastly fewer boys are protected. HPV vaccination rates trail those of other recommended adolescent vaccines, and with evidence mounting that HPV causes a number of different cancers in both men and women, physicians and public health officials are perplexed.
A recent study published in the journal Pediatrics shows that more parents are refusing to vaccinate their adolescents against HPV than they were five years ago. “That’s the opposite direction that rate should be going,” says Dr. Robert Jacobson, a pediatrician with the Mayo Clinic and co-author of the study.
A recent analysis from the Centers for Disease control and prevention showed that even though far fewer teens have been vaccinated than expected, HPV rates among teenaged girls (aged 14-19) dropped by 56 percent between 2007 and 2011.
HPV is the most common sexually transmitted infection in the United States. According to the National Cancer Institute, over half of the people in the U.S. are infected with one or more types of HPV during their lifetimes. In the majority of cases, the infection clears up on its own. But, in a small percentage of people, the virus takes hold and causes cellular changes that can lead to cancer.
This year, there will be 22,000 new diagnoses of HPV-related cancers in the U.S. Thirteen thousand will be cases of cervical cancer; of these, 4,000 women will die. The other 9,000 HPV-related cancers include cancer of the genitals, anus, mouth and throat.
“We know that cervical cancer still does kill people in the U.S., and it certainly causes morbidity because of procedures that people need,” says Dr. Maria Mead, medical director of the Santa Cruz Women’s Health Center. “We see many people go through procedures such as cone biopsies [where a large amount of tissue is removed from the cervix], which can lead to high-risk pregnancies.”
She adds, “With the vaccine, we should see fewer of these procedures and less need for pap smears and surveillance for these cancers.”
When the first HPV vaccine, Gardasil, came onto the market in 2006, public health officials thought they would live to see cervical cancer follow the path of polio—that through vaccination the pathogen causing the disease would become so rare, it would essentially cease to exist.
“We had this wonderful vaccine that was close to 100 percent effective in preventing the two strains of HPV that cause 70 percent of cervical cancer cases in females,” says Dr. Jacobson. “The focus was on vaccinating all eleven-year-old girls in the country. But we failed.”
By 2011, only one in three adolescent girls in the United States had completed the three-dose series they need to achieve full immunity from HPV infection. This low rate prompted public health officials to recommend that boys be vaccinated too, in order to decrease exposure to girls.
“Originally we thought we were just protecting women.” explains Dr. Jacobson. “But as the decision was made [to start vaccinating boys], studies were finalized that showed there may be 9,000 new HPV-related cancer cases in the United States each year that are shared by both women and men involving the genitals, anus, throat and mouth. Now we have good evidence that the vaccine protects both men and women.”
California’s HPV vaccination rate is higher than the national rate—but still far from the U.S. Department of Health and Human Services’ Healthy People 2020 target of 80 percent coverage.
“The coverage is higher among Hispanic girls in California, which is counterintuitive to what you’d expect to see,” says Dr. Diana Ramos, board member for the California Medical Foundation Association. While 51.8 percent of Latinas were fully vaccinated in 2011, only 34.1 percent of white girls were.
Dr. Ramos attributes the higher rate of coverage among Latinas to public health outreach towards a population with a disproportionately high rate of cervical cancer. In addition, low-income children in California are disproportionately Latino and eligible to receive free vaccinations.
There is evidence that the HPV vaccination, albeit at a lower than desirable rate, has already had an impact in the number of genital wart infections in California. A study looking at public health data between 2007 and 2010 found that the number of genital wart diagnoses decreased 35 percent and 19 percent in females and males under the age of 21, respectively.
Still, Dr. Jacobson maintains, “We’ve got a long way to go before we can achieve the uptake we need to make a difference in cancer rates.”
Part of the problem is the nature of the vaccine. Since full immunity requires three vaccinations over a six-month period, busy parents and teens often neglect to return for follow-up appointments. But more worrisome to Dr. Jacobson is the trend he’s seen in his research, where more parents are refusing the vaccination for their children.
In 2008, 5 percent of parents surveyed nationally were concerned about safety of the HPV vaccine. In 2010, the number of parents concerned about safety rose to 16 percent. Less than 1 percent worried about the safety of other adolescent vaccines.
Yet during the same time period, the safety and efficacy of the HPV vaccine was proven in numerous studies. The most common side effects are mild infection at injection sites and a risk of fainting—both of which are likely a reaction to getting a shot, rather than caused by the vaccine itself, says Dr. Jacobson.
He believes that safety concerns are more telling of parents’ real dilemma with the vaccine: it’s an immunization for a sexually transmitted infection. “Here we are in 2013 with stronger than ever evidence that there is a need for the vaccine, but parents think their child is not going to be the sort who gets a sexually transmitted disease.”
The reality is that anyone who is sexually active in the United States has a 50% chance of acquiring an HPV infection, says Dr. Jacobson. That means a child could wait until marriage to have sex and still become infected from his or her spouse.
And the HPV vaccination is not a morning-after shot. If someone already has an infection, it’s not effective. That is one of the reasons that the CDC recommends vaccinating children at 11 or 12—though the vaccine can be given to children as young as 9. In addition, studies show that preteens and young teens have the strongest antibody response to the HPV vaccine.
“The body’s immune system is at its very best at 9-11 years of age,” explains Dr. Jacobson. “We can start as early as 9 years old to really take advantage of that wonderfully vibrant immune system that really responds to the vaccine.”
In 2012, it became legal in California for adolescents to receive the HPV vaccination without parental consent. Still, transportation and other logistical hurdles make it difficult for many to actually do so.
“Occasionally parents will reject the vaccine and their kids will come back later to get it,” says Dr. Mead. “I tell parents that it has nothing to do with whether your child needs it now. The vaccine is more effective if we give it earlier—and it’s protecting them for later.”






You must be logged in to post a comment.