Medically fragile children belong at home with their families, not in institutions. To make that possible, these children need support, especially if they depend on life-sustaining medical equipment such as ventilators, IVs or feeding tubes. In the hospital, these children receive round-the-clock care from doctors and nurses. At home, they still need nursing care.
But a critical program that medically fragile children depend on to get at-home care is broken, leaving families desperate. This is a medical and developmental emergency for children with disabilities, and California needs to act quickly to fix it.
California has some of the most robust programs to support kids with disabilities who are living at home. Kids who are eligible for Medi-Cal, California’s health insurance program for low-income families and people with disabilities, can access private-duty nursing care, medical day care programs, paid family care through In Home Supportive Services, and specialty care through California Children’s Services. Private health insurance — the kind that people have through employment — doesn’t pay for long-term care. Medi-Cal is the only program that pays for the kind of care that medically fragile children need to live at home. California has a waiver program that allows these children to access Medi-Cal. The problem is, it’s full. That means children who need access to this program are languishing on a waitlist instead of getting the care they need.
This is rationing and discriminatory — the state has made a budget decision to ration the care that disabled people need to live at home. There is no moral defense for this kind of rationing. We can’t call ourselves a progressive state if medically fragile children and adults can’t get the care they need to stay out of institutions.
Waivers are a way for states to provide extra services to people who have special care needs, or to provide Medi-Cal eligibility to people who wouldn’t otherwise qualify. For disabled, medically fragile children, the Home and Community Based Alternatives (HCBA) Waiver allows middle-class children to access Medi-Cal programs, like home nursing care.
On July 12, the state announced that the HCBA waiver was at capacity, and that any new applications would be put on a waitlist. The program has a capacity limit of 8,974 people — that means that in a state of 40 million people, a tiny fraction (.02 percent) of people can access it. As of September, there were 3,233 people on the waitlist. What does it mean to be on the waitlist? It means that instead of getting care, the state puts your name on a list of people who need care. There are rules in place that bump medically fragile children to the top of the waitlist — but that isn’t a real solution. The solution is that there shouldn’t be a waitlist at all.

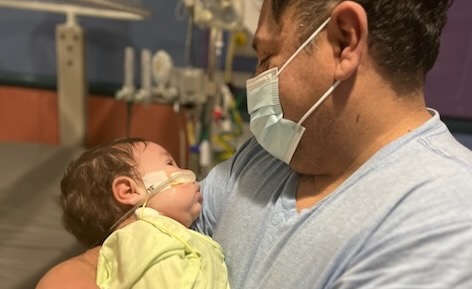
Michelle Zapata‘s 15-month-old son Oliver is one of the medically fragile children who is locked out of getting the care he needs because he’s on the waitlist. Oliver was born with a complex heart defect that couldn’t be surgically corrected until he was 7 months old. Even after the surgery, the defect is not fully resolved. He still needs medications to keep his heart from working too hard. He came home from the NICU at 2 months old, with a feeding tube and a need for round-the-clock feedings and medications to manage his heart condition.
When Oliver came home from the hospital in 2022, the waiver was functional — but he fell through the cracks. No one at the hospital told Michelle that her son qualified for private duty nursing care or the waiver. This has been a longstanding problem with the program — even during the years the waiver was functional, it was a tiny program that wasn’t well connected with hospital discharge planning teams. If the hospital had referred Oliver to the program when he left the NICU in 2022, he would have been enrolled while it was still operational. Michelle learned about the waiver through an acquaintance and applied in August of 2023, after the program stopped taking new enrollments.
Michelle works as a nurse practitioner and her husband works for the government. They’re a middle-class family with private health insurance — but their health insurance doesn’t pay for private duty nursing care. That means Michelle is responsible for all of Oliver’s complex medical care.
“I’m a bedside nurse 24/7 with my son, (and) on top of that I have my own job,” she told me.
Without nursing help at home, Michelle has to rely on Oliver’s grandparents for help so that she can work. Oliver’s grandmother accidentally gave him too much medication one day — 7 mL instead of 0.7 mL — because the labels, syringes and instructions all had very small print. Medication errors are an easy mistake to make, especially for people with no medical training taking care of a fragile infant. Thankfully, Oliver was O.K. – but he still doesn’t have access to the professional nursing care he needs to reduce the risk of untrained family members making future errors.
If Oliver could enroll in the waiver program, he would also be able to attend Loretta’s Little Miracles, a pediatric day health program where nurses take care of kids who have complex medical care needs.
The irony of the situation isn’t lost on Michelle. “I work in health care — I work in the system that I can’t even get access to,” she told me.
For Oliver to qualify for Medi-Cal without the waiver, Michelle and her husband would have to quit their jobs, which would be economically disastrous for the family.
This dysfunction in the HBCA waiver program comes at an especially dangerous time for medically fragile children. During the COVID-19 public health emergency, children remained eligible for Medi-Cal even if their parents didn’t complete renewal paperwork. Then in April, California restarted Medi-Cal redeterminations, which means that families who are over the income limit to qualify without a waiver will be disenrolled. Some of these families have children who are receiving private duty nursing care without a waiver, because they qualified for Medi-Cal when their incomes were lower. Normally, if their child has a serious disability, they’d still qualify for home nursing through the HCBA waiver, even if their income has increased. But because of the waiting list, they’ll instead lose access to care. This could force parents of medically fragile children to drop out of the workforce to take care of them, or to choose unsafe care arrangements that put the child at risk of injury or death so they can keep working. Parents with no other options may have to make the devastating choice to put medically fragile children into institutional care.
This crisis doesn’t just affect medically fragile children.
Adults who need nursing care at home are also on the HCBA waitlist. The HCBA waiver is a true lifespan program: it provides care for ventilator-dependent infants, toddlers who use parenteral nutrition, children who are on peritoneal dialysis pending kidney transplants, teenagers with muscular dystrophy, young adults who have been paralyzed, adults with ALS and other neurological syndromes, and elderly people with dementia. Right now, the HCBA waiver is a zero-sum game — the people on the waitlist are waiting for people currently enrolled in the program to die in order to get care. The state is supposed to have a “triage” process for the waitlist that prioritizes some applications over others, but the rules on how that will work and when enrollments will restart haven’t been released. Disabled people who need care are drowning, we shouldn’t have to agonize over who gets a spot on the lifeboat — we can build a bigger boat.
California doesn’t put a limit on how many sick people can get care in hospitals or nursing homes. California has a similar waiver program for people with developmental disabilities called the Home and Community Based Services – Developmentally Disabled (HCBS-DD) Waiver, which doesn’t have a capacity limit. But for complicated budget reasons, California sets a limit on how many children and adults with medically intensive disabilities can get nursing care at home, and it’s a very low limit.
It also makes no economic sense. Warehousing disabled people in hospitals and nursing homes costs the state orders-of-magnitude more than just providing nursing care at home. When vulnerable people can’t access nursing care at home, the state spends millions on unnecessary hospitalizations.
The state has committed to providing enhanced case management and community supports for people who are at risk of institiutionalization or trying to come home from an institution. But with the HCBA waiver at capacity, California’s promise of wraparound services for the most medically complex patients is hollow.
California can fix this by immediately funding 50,000 slots for the HCBA waiver and eliminating ongoing capacity limits. This isn’t a problem that can wait until the next budget cycle for a solution. Californians who need care today can’t get it. Families are having to make gut-wrenching decisions: Do their children stay in the hospital, where they have access to medical care but not family life, or do they bring them home without adequate support? Waiver capacity is set to increase to 10,081 slots in January of 2025 (or perhaps sooner). That’s not enough capacity to handle the people who are currently on the waitlist, or the people who will apply between now and then.
California has made an indefensible decision to ration the care that its most vulnerable residents need to live at home. The rationing needs to stop now.

Jennifer McLelland has a bachelor’s degree in public policy and management from the University of Southern California and a master’s degree in criminology from California State University, Fresno. She worked for the Fresno Police Department in patrol for eight years. She is currently a stay-at-home mother and paid caregiver through the In Home Supportive Services program. She is active in advocating for disability rights and home- and community-based services.






You must be logged in to post a comment.